MACRA Monday: Quality Performance Category

MACRA Monday: Quality Performance Category October 24, 2016
Every Monday for the next four weeks, we’ll be breaking down the four performance categories that independent practices will be required to report on when MACRA and MIPS goes into effect on January 1.
An estimated 90% of eligible providers participating in the Medicare Access and CHIP Reauthorization Act of 2015 (MACRA) will be subject to MIPS — the Merit-based Incentive Payment System. As we’ve previously explained, MIPS has four performance categories that will be used for the MIPS Composite Performance Score (CPS) that determines these new value-based reimbursements. CMS (Centers for Medicaid Medicare Services) recently finalized the way these categories will be weighted:
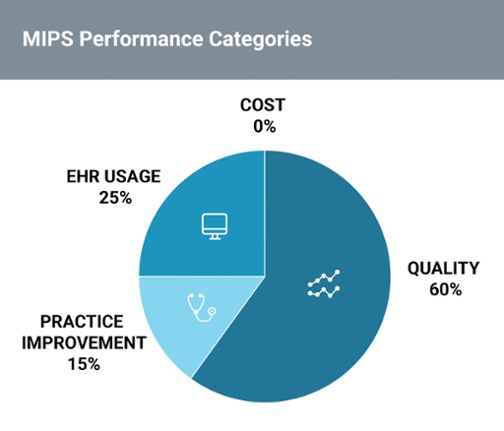
With MACRA as a broader push toward value-based and quality care, it’s not surprising “quality” constitutes the largest performance category. In order to attest for quality, practices now have options for how they would like to participate in MACRA during its first year.
What are the requirements?
Many providers might choose to prolong their full-participation and simply submit minimal quality-related data. For the MIPS eligible physicians that would like to fully participate in the program come January 1, providers will have to report on at least six measures, including at least one outcome measure if applicable. In some cases, fewer than six measure may apply to a provider or group, and in such a case, the provider or group will only have to report on each relevant measure.
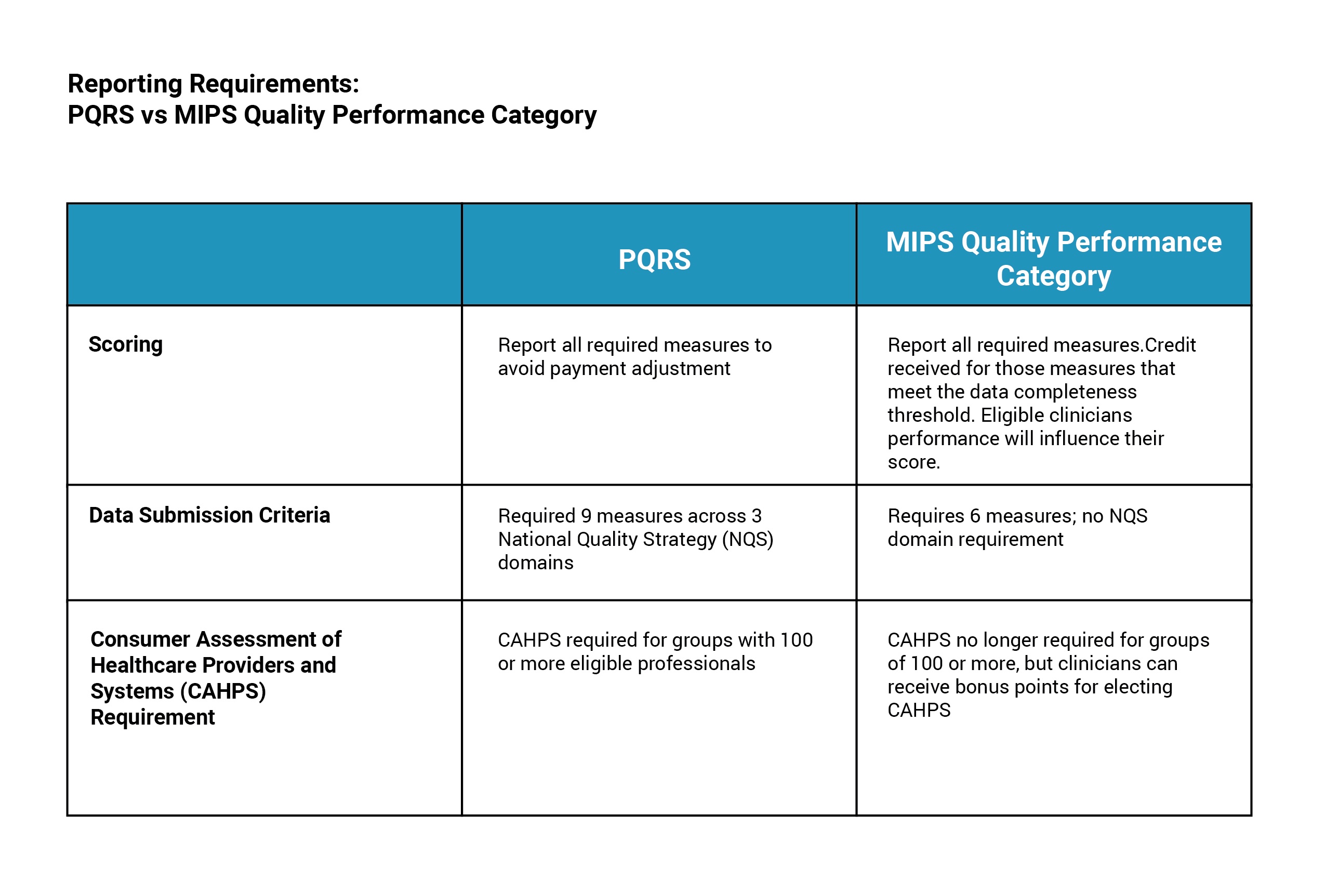
How is the MIPS Quality Performance Category different than PQRS?
As a small or solo practice physician, you may be familiar with the Physician Quality Reporting System or PQRS. Starting in 2017, after MACRA kicks off, the Quality Performance Category will replace PQRS.
How will the quality measures be selected?
CMS expects to equip physicians and practices with a pool of 200+ measures that you can choose to report on. According to the final rule, “Quality measures will be selected annually through a call for quality measures process, and a final list of quality measures will be published in the Federal Register by November 1 of each year.”
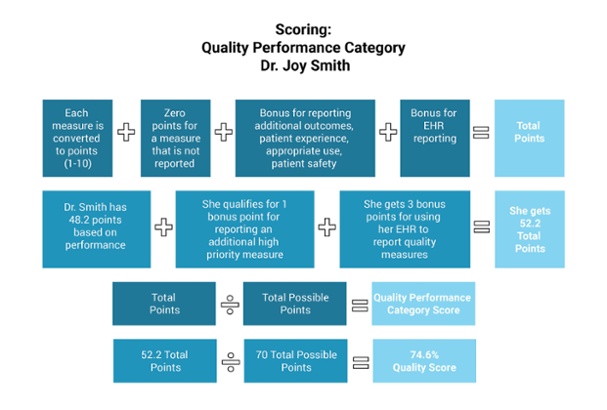
How is the quality score calculated?
The quality score is calculated by combining points for each reporting measure with bonus points for patient outcomes and EHR reporting. A primary care provider in a solo practice, like the example provided below might calculate her score like this:
Key Takeaways:
• Quality is the largest reporting category for MACRA/MIPS and replaces PQRS.
• Independent providers have options for how they would like to participate during the first year of MACRA/MIPS.
• Providers that are ready to jump into MACRA in 2017 should be prepared to report on about 6 measures out of the 200+ measure options, depending on which measures are applicable to their practice.
Subscribe to our MACRA Resource Series to recieve content like this straight to your inbox!
![]()






