Avoid 2019 MIPS Penalties by reporting on 1 patient for 1 measure

Avoid 2019 MIPS Penalties by reporting on 1 patient for 1 measure December 29, 2017
As the first year of the Merit-based Incentive Payment System (MIPS) track for MACRA comes to a close, many physicians participating in the program might be wondering what action they need to take to avoid costly penalties. With Elation’s built-in dashboards and health policy support, you can put your stresses at ease and avoid penalties in 2019, as a result of performance in 2017.
How do you report for MIPS in 2017?
The Centers for Medicare & Medicaid Services (CMS) recently loosened some of the requirements of the program. These requirements mean 2017 is a transition year for MIPS and the minimum practices need to do is report some data to test the program and avoid penalties.
To avoid 2019 penalties, all you need to do is report on 1 patient for 1 measure.
How to do you know which measure to select?
Check your CQM dashboard to see which measure you can report on! If you have 1 patient who meets the numerator and denominator for any measure, as long as you report that data point, you will avoid penalties. To access the dashboard, go to the “Reports” section in Elation.
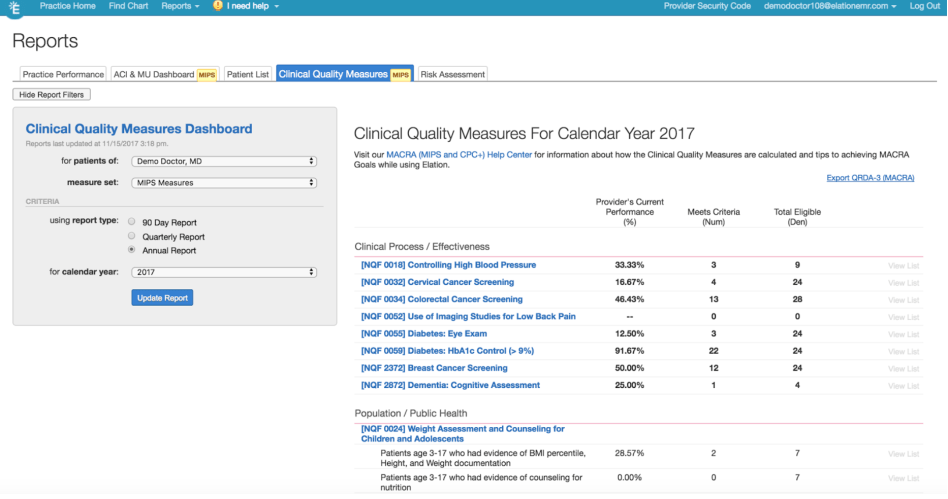
Identify which measure is best for your practice by reviewing our CQM webinars below:
