During the Pandemic, Mission and Margins Collide in Independent Primary Care

Dr. Manvinder Kainth worked in large hospitals for a decade before she decided to open her own practice in Texas. It was a difficult decision, but it stemmed from a simple belief: The American healthcare system wasn’t treating patients or doctors like their health was its top priority.
As the coronavirus pandemic puts unprecedented pressure on healthcare, flaws are exposed that lend credence to Dr. Kainth’s belief. Physicians go to work without proper personal protective equipment. Hospital leaders prohibit healthcare workers from speaking to the press about dangerous working conditions. Some doctors face pay cuts, precisely when their service is needed most. Too many people — doctors and patients — are dying from preventable deaths.
These daunting facts don’t surprise Dr. Kainth, but that doesn’t make them any easier to stomach. “I am angry that the hospital system didn’t react more quickly,” she says. “It’s because hospitals are not run by doctors. They’re run by businessmen and women. And I have a lot of anger toward that.”
This type of disaffection and disillusionment is common among physicians who have worked in hospital systems and made the leap to independent practice. But independent practitioners are anything but pessimists — in fact, they bubble with excitement and pride when asked about the relationships they’ve built with their patients.
Many say that independent practice helped them rekindle their deep-seated passion for medicine. Like nothing else, practicing independently gives them personal and professional purpose.
Now, however, as the pandemic bears down on their businesses, independent primary care physicians’ passion and purpose are in jeopardy once again. Having escaped the system that prevented them from living out their dreams, coronavirus forces them to face new technical, financial, and ethical challenges that threaten to undermine their way of life and wreak havoc on the patients who depend on them to stay healthy.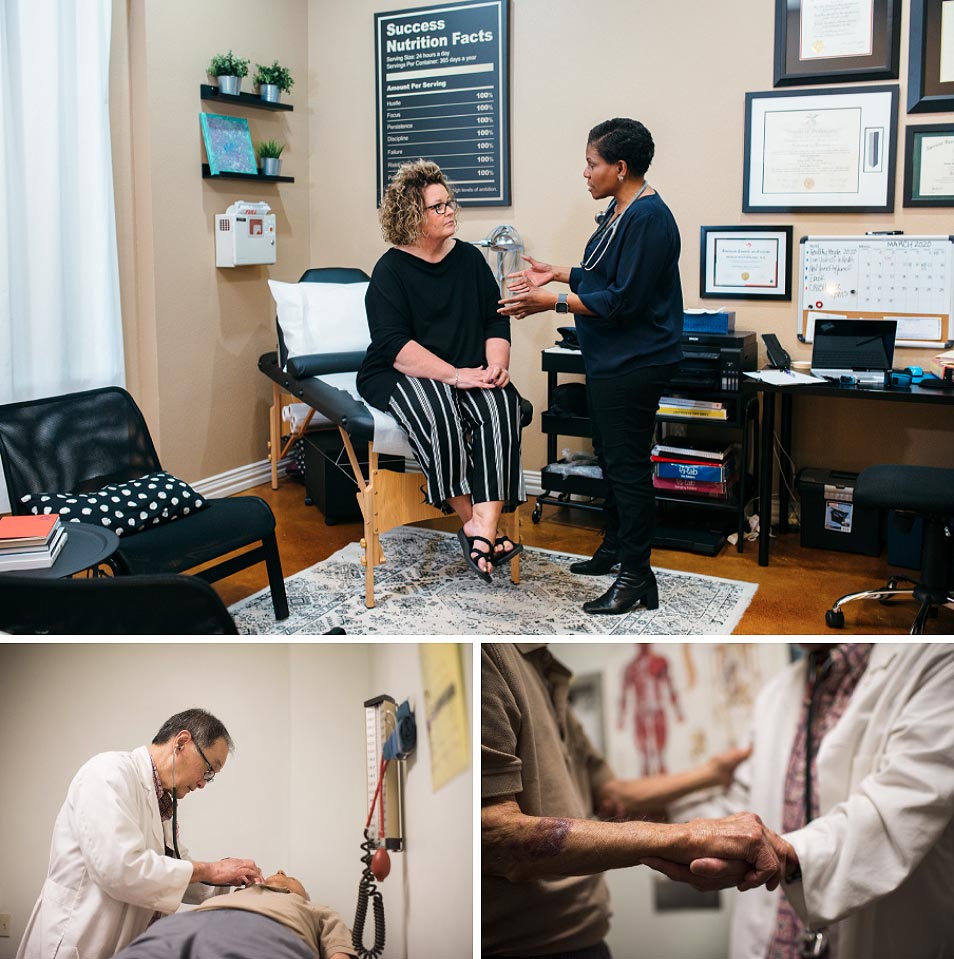
How Do I Adapt?
Dr. Kainth practices under a unique business model called direct primary care, or DPC for short. While the care system is not widely known, members of the DPC community tend to evangelize its benefits, pointing to improved patient-physician relationships, greater focus on patient and physician satisfaction, and reduced costs as cornerstone elements of the practice.
Unlike the fee-for-service payment model leveraged by many large health systems, which incentivizes churning through patient visits rapidly in order to increase revenue, DPC doctors typically charge a flat monthly or annual fee that entitles their patients to communicate with or visit their provider as often as they’d like.
Longer and more frequent appointments help build trust, strengthen community bonds, and establish a culture of reciprocal support, according to Dr. Natalia Southerland, a DPC physician who opened her own practice, called Brand New Med, in Waxahachie, Texas, nearly three years ago. But when social distancing rules swept the nation and independent practices moved to nearly 100 percent virtual appointments via telemedicine and other digital means, Dr. Southerland found it difficult to deliver value like she could before. “I guess I’m just really old school,” she says. “I feel better when I see people in person.”
Still, Dr. Southerland accepts the necessity of delivering care virtually during the pandemic. Most patients have warmed up to it as well, but many, including the technology-averse and elderly, are having a tougher time. The challenge is exacerbated by technical problems, which, according to Dr. Owen Nishikawa, an independent primary care physician in Honolulu, Hawaii, have put a dent in the way doctors maintain connection with their patients. “There are always these unexpected things where the telemedicine system is down, or the patient isn’t able to sign in, or there’s some glitch,” he says. “This has come up a number of times, so even though we have appointments set up, we’re not always able to carry through with them.”
Dr. Nishikawa believes once the wrinkles are ironed out and patients become more comfortable with the service, telemedicine holds the potential to help doctors uphold better office hygiene and improve care delivery to underserved communities. Until then, he sees it as a small part of a temporary mitigation strategy to help his business stay afloat and avoid losing touch with patients.
Although independent primary care doctors are seeing patients less often, they’re fielding more questions from nervous patients. Data pulled by Elation Health, an electronic medical records provider, shows that independent primary care practices are managing a 60 percent increase in messages from patients. “It’s allergy season, so everyone is calling with a cough,” says Dr. Neha Doshi, a concierge primary care physician in Winter Park, Florida. “Lots of people think they have COVID-19. I know it’s my job to educate, educate, educate.”
That education is a huge part of quality care, especially during a pandemic, Dr. Doshi explains. First, arming patients with facts increases the likelihood that those facts will be shared with other patients. Second, the information might prevent them from running to the emergency room at the first sign of sickness and adding unnecessary burden to health systems.
“Let’s talk every day,” Dr. Doshi advises concerned patients. “Text me, call me. Let’s be in close contact while you stay safe at home.”
Dr. Doshi’s high-touchpoint approach is common among independent practitioners, who often consider their patients’ well-being and peace of mind a measure of their own professional success. But as coronavirus spreads, workload increases, and visits plummet, doctors are facing another challenge.
Receiving more messages is “good because [doctors] are able to help patients virtually,” wrote Elation Health Founder and CEO Kyna Fong, in a tweet. “It’s bad because they are paid almost nothing for these touchpoints.”
How Do I Stay Solvent?
In independent practice, physicians are empowered to set up custom reimbursement models that align with their values. In DPC, most doctors use flat monthly or annual fees. It’s like a handshake between a physician and their patients that acknowledges their interdependence — DPC physicians depend on patients to support their businesses, and patients depend on DPC physicians to support their health.
The model’s simplicity attracts many who don’t have insurance, like those who work in retail, service, and gig positions. But a model based on monthly fees only works as long as patients can continue paying. As social distancing rules prevent many Americans from heading to work, they’re forced to face difficult questions about the wisest ways to spend.
“I’ve seen about a 10 percent reduction in memberships,” Dr. Southerland says, explaining that most of this reduction is attributable to patients who’ve been laid off in the wake of the pandemic. “It stinks because morally, you know these people might not be getting help at all. A lot of times they’re not well off financially, and they are chronically ill, too. On top of that, it really hurts your bottom line.”
Dr. Southerland is toying with different ways to make up for the losses. She’s applied for several government loans and has even discussed forbearance and altered payment plans with some patients. But these are temporary solutions. If the pandemic continues to push her patients out of work and prevent them from paying for care, it’s unclear how she’ll keep her business afloat.
Dr. Kainth is in a similar position. Memberships at her practice have plummeted by about 20 percent. Like Dr. Southerland, she’s working to secure government loans and trying to stay flexible as her unemployed patients balance physical and financial needs. Beyond that, “I just take it on the chin. There’s not much more I can do as far as changing things around,” she says. “I’m not upset with my patients’ decisions. I completely understand. Those are just the crappy circumstances that we’re all in right now.”
The future remains uncertain even for independent physicians who rely on insurance payments. Dr. Nishikawa is reimbursed based on complex metrics that take into account the number of patients he sees, but also the different diagnoses he makes, patient risk factors, and more. Even after turning to virtual visits to keep lines of communication open with the nearly 2,000 patients that routinely visited his practice before the pandemic, he is still seeing a 50 to 75 percent reduction in appointments. So far, his income hasn’t dipped, but it’s unlikely to remain consistent in the future.
With financial figures in a state of uncertainty, big-picture plans have been thrown into question. In early March, for example, after a year of searching, Dr. Kainth purchased a second property to expand her business. Now, immediately following one of the largest investments of her life, she must rein in spending because she estimates she might lose 40 percent of her patient memberships.
Dr. Southerland is facing a similar conundrum. She recently began renting space in Dallas, where she felt she could gain traction with the younger, professional demographic by opening a health coaching clinic. She planned a soft launch for mid-April, which has since been pushed to mid-May. Now, Dr. Southerland worries over the financial futures of two businesses and wonders whether the clientele she is targeting — in Dallas and Waxahachie — will have enough disposable income to support the next evolution of her business by the time the pandemic subsides.
“These independent primary care practices are putting their own health and financial futures on the line to do what is right for their patients during #COVID19. They’re answering phone calls, visiting patients, taking care of the highest-risk and elderly,” Fong wrote. “Primary care provides critical front-line capacity for triage, outbreak detection, and managing chronically ill patients who struggle even outside of this pandemic. Especially the independent practices working in areas where there’s the least patient access to care.”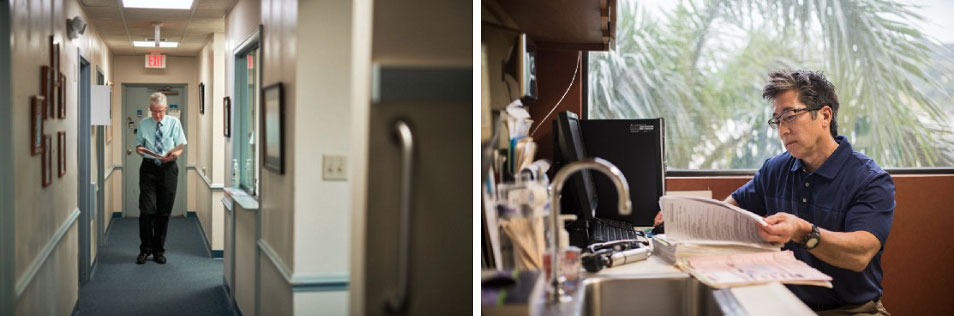
How Do I Make a Difference?
Independent primary care doctors know that there’s no mission without a margin. But “most of us did not go into our profession to make the big bucks,” Dr. Kainth explains.
Purpose is primary, and for many physicians, that purpose lies somewhere between giving their all to patients and building relationships that matter.
As COVID-19 bears down on the nation, purpose remains top of mind, but the steps needed to achieve it have changed. Meaningful relationships are a bit harder to build and sustain virtually. Giving your all to patients by telling them to stay at home can feel anticlimactic. Behind these moral difficulties lingers the ever-present specter of insolvency. Suddenly, for many physicians, independent practice is beginning to carry many of the same stressors of employment.
“I do a really good job. I’m a really good doctor. If you go to my Facebook page, you’ll see people saying, ‘She really is the best doctor I’ve ever been to,’” Dr. Southerland explains. “But that’s just not enough. That’s not enough anymore. People keep telling me that patients should be flocking to me, but it’s just not happening.”
Bills continue to arrive without fail, but payments from patients are beginning to slow.
The values that empowered Dr. Southerland to withstand 20 years of challenges at health systems and conjure up the courage to make the leap to independent practice haven’t wavered, but out of necessity they’re starting to take a back seat to financial concerns.
Measures that would be out of the question were it not for the pandemic are beginning to resemble foregone conclusions — letting staff go, firing long-standing and mutually supportive small business clients, even cutting ties with cleaning staff and spending hours scrubbing down the office by yourself each week aren’t out of the question.
If the pandemic pushes her much closer to potential insolvency, Dr. Southerland is mulling another exit — this time, from medicine altogether. “It hurts my heart to say this, but I don’t know that this is going to sustain me or make a difference. Financially, I would need a windfall of patients to come in here,” she says. “My work isn’t done, though. I’m still going to be helping people. I might just move it all to health coaching, so I can teach people a different way of life and help them change for the better. To me, that’s more important than anything.”
While the future remains unclear for independent primary care doctors, what’s certain is that they provide value to society far beyond what can be measured economically.
They’re consistent sources of reliable information during a pandemic where falsehood seems to make the rounds with unprecedented speed, causing unknowable harm. They’re frontline triage workers during a time when hospital systems are buckling under the pressure of the worst pandemic in generations. They’re a comforting, accessible voice during a time when we all confront the challenge of isolation, fear, and uncertainty. And they represent access to care for millions of underinsured patients, many of whom struggle to make ends meet while providing services society deems essential.
It would be a tremendous failure for society to use taxpayer funds to prop up nonessential businesses and their well-to-do owners while allowing independent primary care offices to sputter toward financial ruin. Changing times necessitate changing priorities. During this pandemic, we must prioritize the sustained operation of independent primary care offices not just for their own sake, but for their patients and the value these doctors provide to society.

