How This Direct Primary Care Physician Is Earning Patient Trust
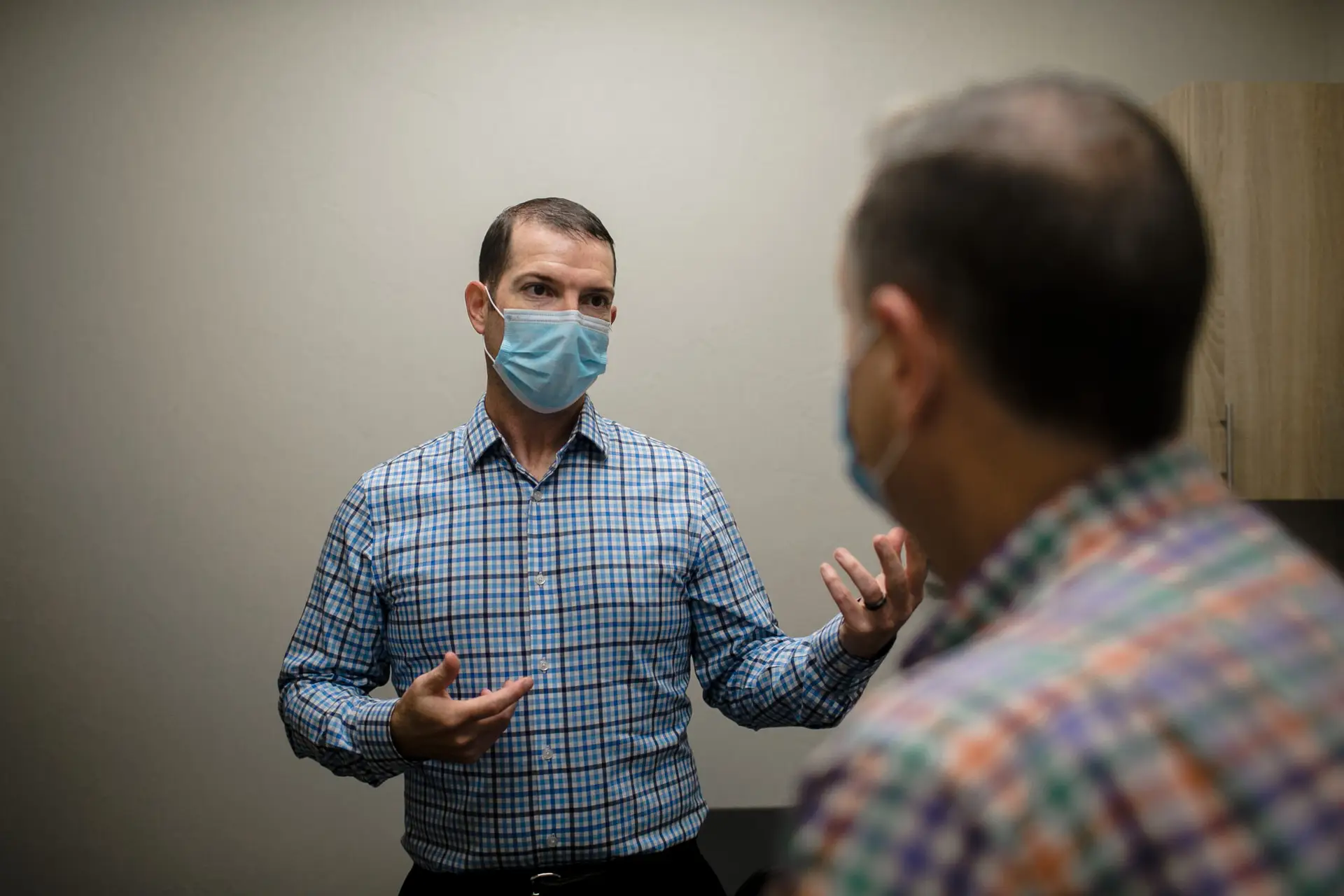
Dr. Jonathan Bushman was heading somewhere few physicians go: jail.
As he cruised through the summertime streets of Enid, his small Oklahoma city, he was neither anxious nor afraid. After all, this wasn’t his first trip behind bars. But Dr. Bushman has never served time — he just treats those who are.
For the past two years, he’s been caring for the inmates of two county jails, a job he took not knowing what to expect. Soon, he saw a revolving door of patients, some of whom had committed terrible crimes and many who had a “survival mentality” with a distrust of everything, including medicine. Many of his patients didn’t even have access to care when they were on the streets.
Dr. Bushman yearned to help them. But how could he earn inmates’ trust so that he could provide care they might not get elsewhere? He chose a simple strategy: Treat them like he would the hundreds of patients enrolled in his direct primary care practice.
Nurturing patient trust
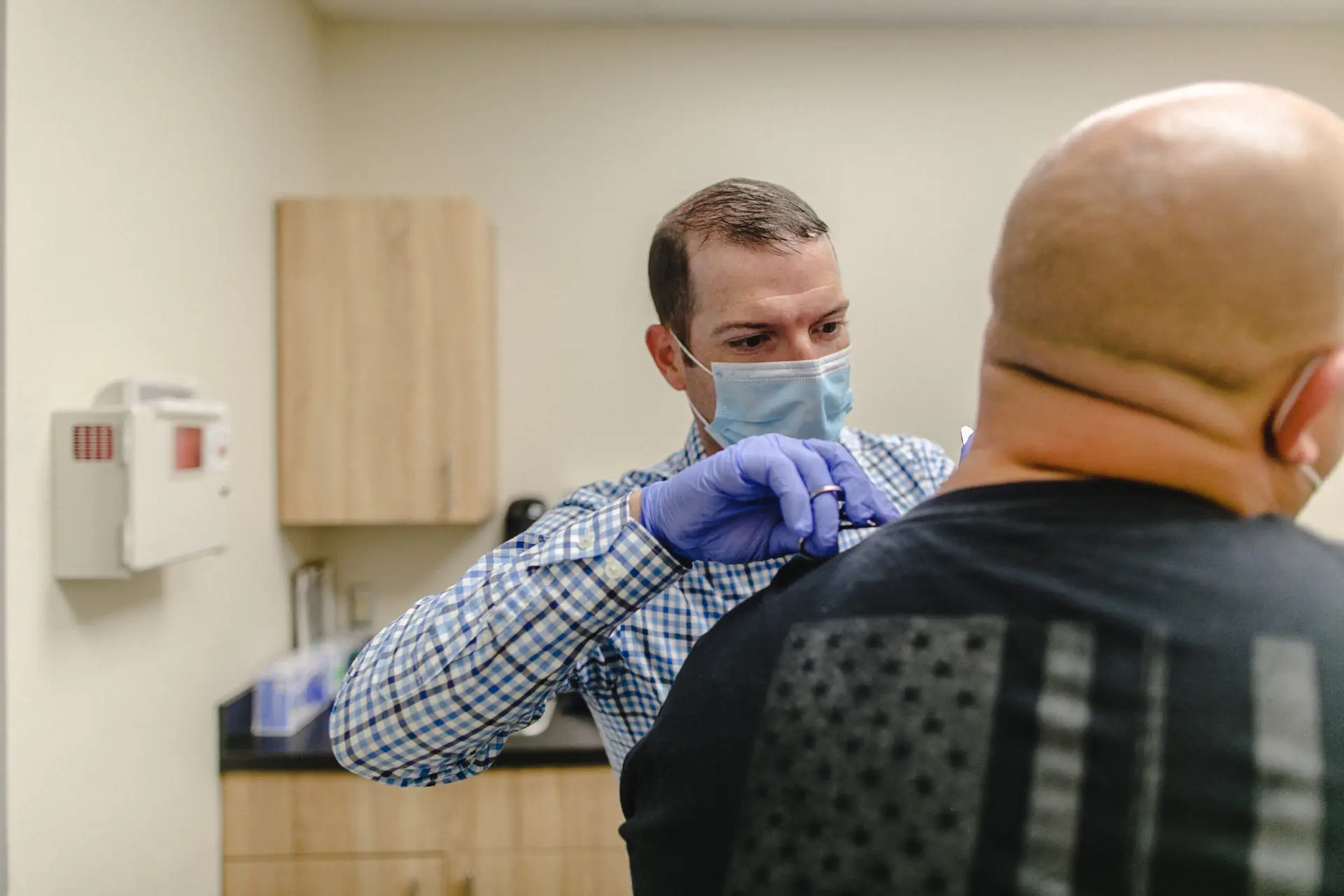
“I’m not your priest. I’m not your parole officer. I’m not a police officer. I’m your physician, and my responsibility is to take care of you,” Dr. Bushman tells his incarcerated patients. “These walls don’t make a difference in that, just because you’ve done something to hurt someone else or yourself.”
Medicine rarely draws comparisons to life on a cellblock, but these two different corners of the universe have one thing in common: Trust is tough to attain.
Direct primary care allows me to focus on who should be at the forefront of every conversation, which is the patient.”
Perhaps that’s why Dr. Bushman, a husband and father of three who studied political science in undergrad, approaches medicine almost like a community organizer. To help patients achieve good health at a reasonable cost, he has worked to build trust in almost every way imaginable. From the moment he started his direct primary care practice, for instance, he launched a campaign to inform patients how a relationship free of insurers would benefit them. He made house calls. He joined Oklahoma’s medical association and local leadership groups to contribute to big-picture solutions. He agreed to treat his community’s most vulnerable patients, inmates, without flinching.
“If I leave any sort of a legacy within my profession, I hope it’s that I held that relationship at the very highest of my priorities,” Dr. Bushman says. “I can’t rid my patients or myself of the world of big pharma or Medicare or all of those third parties. They’re still there in some way, but at least direct primary care allows me to focus on who should be at the forefront of every conversation, which is the patient.”
A wake-up call to vulnerabilities in the healthcare system
But before he won over his patients, he had to revive his own faith in healthcare.
Dr. Bushman’s distrust in the system skyrocketed when he became the patient. He was working for a large self-insured health system and needed an MRI scan. When he dialed a hotline to determine what it would cost him, the voice on the other end fell silent. Dr. Bushman called another number, waited 10 minutes, and learned that he was on the hook for more than $1,000. The health plan didn’t know, or wouldn’t share, the total bill. Irked, Dr. Bushman went to an out-of-network imaging center, where he paid $400 in cash and underwent the MRI on the same day.
He had an epiphany. If health systems and insurers could muddy the financials for a doctor, what sort of deal did patients get? That question turned to introspection. If Dr. Bushman fought so hard to save his own money, why didn’t he do the same for his patients?
“It really hit me hard because I realized I wasn’t working for my patients. I was working for the health system,” Dr. Bushman says. “And that just bothered me. It still bothers me that I’ve almost haphazardly spent other people’s money or employers’ health plan dollars in ways that really didn’t need to be spent.”
The road to direct primary care
Since he began training, Dr. Bushman had slowly grown concerned that hospital administrators were chasing goals that wouldn’t benefit patients. Healthcare was about maxing out the number of patient visits, coding for as many actions as possible, and billing for sport. This incident only worsened the bad feeling in his gut.
Not long after, he was giving a luncheon talk to a group of medical school students. It was basic stuff — the history of medicine, the fee-for-service model, and so on. Toward the end of the lecture, a student raised her hand and asked an unexpected question: Do you ever feel like you don’t have enough time to practice medicine at your best?
“It honestly almost hurt when she asked me that because it’s something I had been struggling with for a while,” Dr. Bushman recalls.
I’m doing what I want to do, I’m doing it for all the right reasons, and that’s a peace of mind that I can’t describe,” Dr. Bushman says. “It’s just a feeling when you know that you’re taking care of [your patients] the best that you can.”
After the talk, the student brought up direct primary care. Her father had run one such practice for years, finding both success and fulfillment. Dr. Bushman was intrigued. He hadn’t only heard of direct primary care, he’d been considering it.
Working for the health system only became more troubling. Dr. Bushman soon told his wife that if it weren’t for two colleagues, he’d be ready to quit and start a direct primary care practice. Two hours later, he got word that not one but both of them had resigned. Dr. Bushman was relieved, almost elated, as he raced home.
He and his wife made a list of the things they’d be willing to sacrifice for the emotional freedom and financial uncertainty of going solo. Outside of their family and friends, they found, there was nothing that was worth staying put.
Over the next several months, Dr. Bushman began recruiting patients, assembling an office, and hiring staff. Everyone’s journey to direct primary care is different, but he gathered tips to help other physicians through the process.
- Prepare to lose patients. Dr. Bushman couldn’t convince everyone to follow him to direct primary care. Some didn’t want to pay, while others, such as those on Medicare, couldn’t. When patients asked Dr. Bushman why their trusted doctor was abandoning them, he felt terrible. But he walked away with 10 to 15 percent of his patients, right in line with expectations.
- Keep it simple. Dr. Bushman believes that the less you can live on, the best you can live on. Independent physicians might not match their previous salaries in year one, or ever, but they might find greater joy in medicine. On the other hand, a doctor can work so much that the pay outweighs that of a general surgeon and the misery intensifies. Direct primary care offers physicians a simpler, more rewarding life. Why not take it?
- Get the right EHR. At the health system, Dr. Bushman often felt like he worked for his electronic health record system. When he tapped Elation Health to serve his direct primary care practice, he finally found an EHR that worked for him. The intuitive software made recordkeeping a breeze, and he quickly came to love its focus on patients rather than billing.
Two years later: a thriving practice

Nearly two years later, Dr. Bushman is satisfied. Period. His practice, Reliant Direct Primary Care, has two offices in northern Oklahoma and three providers who serve no more than 1,000 patients each. Even through the turmoil of the COVID-19 pandemic, Reliant has thrived, thanks in large part to telemedicine.
“I’m doing what I want to do, I’m doing it for all the right reasons, and that’s a peace of mind that I can’t describe,” Dr. Bushman says. “It’s just a feeling when you know that you’re taking care of them the best that you can.”
Some patients don’t have health insurance, meaning the practice is their lifeline, but he tries to make them all feel like VIPs. When someone apologizes for texting late or sharing a detailed story in the clinic, he thanks them for taking their care seriously. When new patients come on, he takes the time to hear them out, review their medical records, and investigate potential issues, which recently led to a cancer diagnosis that would have otherwise been missed. When a man contracts COVID-19 and can’t find a physician willing to see him, Dr. Bushman swoops in and admits him to the hospital just days before complications develop, which saves the patient’s life.
When an alleged murderer is struggling with mental health conditions and diabetes, Dr. Bushman is there, too. Because doctors can’t simply wish for patients’ trust. They have to care for it, one conversation and one jailhouse call at a time.
