The importance of primary care during the pandemic
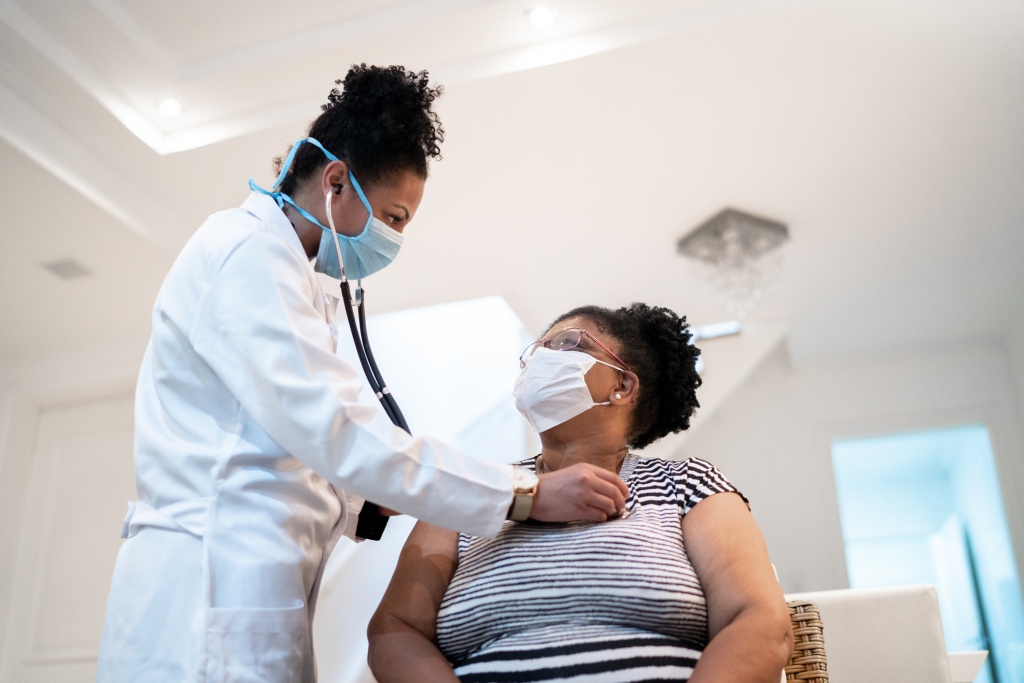
The COVID-19 pandemic has affected virtually everyone across the country in some way. Whether faced with uncertainties about the virus, isolation, financial challenges, or health challenges, individuals have been dealing with pandemic-related issues for almost two years. The importance of primary care during the pandemic has been noted by many experts who see COVID-19 impacting even the health of people not infected by the virus.
When the pandemic began, primary care practices had to suddenly adjust their operations, to either shut down temporarily or shift to telehealth. Once stay-at-home restrictions were eased or lifted, patients returned to the practice on a limited basis while following all appropriate safety guidelines. Individuals suffering from chronic conditions felt the impact of this disruption to their regular care routines, as they were also feeling their vulnerability to complications from contracting the disease.
As the pandemic continues, primary care is essential to the health and well-being of all patients, in many different ways. Primary care delivers the first line of care during the acute phase of a public health crisis. It also helps to maintain the continuity of care for those individuals with chronic conditions. Independent physicians providing high quality primary care services help to reduce the pressure on the entire health system by providing preventive, comprehensive care during and after the health crisis.
The importance of primary care during the pandemic has been shown in the critical role it plays in clinical care, including patient screening and triage, physical and psychological support, and in promoting community awareness coordinated with secondary healthcare options. This role is essential for the short-term and long-term monitoring and care for those affected by COVID-19.
In addition, primary care is the essential foundation for responding to the pandemic as the provider:
- Identifies and triages possible COVID-19 cases
- Makes an early diagnosis
- Helps vulnerable individuals cope with their virus-related anxiety
- Reduces the demand for hospital services.
A pandemic response focused on the importance of primary care has been shown to also be a cost-effective measure, with the increasing role of home care for COVID-19 cases and the closing of hospital outpatient departments. In fact, most people who have contracted the virus develop a mild, uncomplicated illness that can be managed at the primary care level.
Research-based evidence shows that the primary care role during a public health emergency is to maintain essential health services and to respond to the outbreak. The principles of primary care during the pandemic include:
- Maintaining delivery of essential health services
- Identifying and of transmission of infection to contacts and health-care workers
- Enhancing existing surveillance such as for influenza-like illness (ILI) and severe acute respiratory infection (SARI)
- Strengthening riskmanaging potential cases as soon as possible
- Averting the risk communication and community engagement
- Supporting the provision of vaccination services against SARS-CoV-2, the virus that causes COVID-19.
Primary care teams have “faced a tsunami of increasing demands,” write Jennifer E. DeVoe and Andrew Bazemore of the Department of Family Medicine, Oregon Health & Science University in Portland. They have “scrambled to comfort patients, build respiratory clinics, redesign workspaces, develop new protocols, reschedule visits, and interpret still-evolving regulations about scheduling, document, and billing to provide equitable telemedicine services.”
Despite the challenges, DeVoe and Bazemore point out that throughout the pandemic, primary care teams “have kept up on rapidly changing clinical information, ensured timely access to critical therapies, embraced new team-based models of care, engaged patients and families in practice improvement, and rearranged staff schedules when schools closed and waves of COVID-19 rolled through communities.”
Strong primary care, particularly that which is integrated with community health services, equipped with digital technology, and organized with innovative roles for providers and their clinical staff, helps deliver a successful response to the crisis created by the pandemic. These innovations will help to make healthcare more resilient against future public health emergencies, as well as being better able to meet the challenges of an aging society and the growing prevalence of chronic conditions.
